- Vaccination against Covid-19 and Influenza in Switzerland: Perceptions and Attitudes
Introduction
Viral respiratory diseases inflict a significant burden on the health care system in Switzerland. In the 6 hospitals that participated in the CH-SUR hospital surveillance (now discontinued), 1652 people were hospitalized with influenza and 3484 people were hospitalized with COVID-19 in the 2023/24 season (1). In these 6 hospitals, there were 70 deaths with influenza and 246 with COVID-19. Almost 80 % of hospitalized people were above the age of 65 (1), underscoring why this age group is designated as “high-risk population” for COVID-19 and influenza by the Swiss Federal Office of Public Health (FOPH) and the Federal Commission for Vaccination (Eidgenössische Kommission für Impffragen, EKIF) (2, 3). Several hospitals in the canton of Vaud had to postpone elective surgical procedures during the winter of 2024/2025 (4). As vaccinations have shown to be a major preventive factor against hospitalizations and a severe course of the disease (5, 6), the FOPH and EKIF are currently recommending annual vaccinations against influenza, COVID-19 (both over the age of 65 years) and also respiratory syncytial virus (RSV, from the age of 75, or 60 years with specific comorbidities) since 2024. Despite the broad EKIF recommendations (3), widely available vaccines (7), and extensive public campaigns by the FOPH, vaccination rates are very low in Switzerland: While the target of the World Health Organization (WHO) is to vaccinate 75 % of the at-risk population, the estimated annual influenza vaccination rates in the at-risk population are only between 18–39 % in Switzerland and on average 45.7 % in the European Union (8–12). For COVID-19, vaccination rates in the at-risk population in Switzerland are estimated to be even lower, at a maximum of 18 % in 2023/24 and 12 % in 2024/25 (estimated vaccination rates based on data from the following source: (13)). Similarly, the median coverage in the EU in > 60-year-olds is at 14 % (14).
To better understand the reasons behind the low vaccination rates in the at-risk population in Switzerland, we conducted a survey following the 2023/24 season, investigating current perceptions and opinions from both health care professionals (HCPs) and the at-risk population (people from the age of 65 years) regarding annual vaccinations. The results aim to contribute to a better understanding of vaccination attitudes in both HCPs and the general population to develop better strategies to address existing knowledge gaps.
Methods
Study Design
This study was initiated, designed and funded by Moderna and was performed in adapted versions in several countries. Only the outcomes from participants in Switzerland are analyzed and presented here. The study included two parallel online surveys targeting 1) HCPs including general practitioners (GPs) and pharmacists, and 2) individuals aged ≥ 65 years (at-risk population, further referred to as patients) throughout Switzerland. The surveys were conducted in collaboration with the market research provider Dynata, an online digital collection company based in the United Kingdom, which has panels with active respondents around the world (consumer, B2B, patients, and HCPs) (15). Dynata utilized its proprietary online panels for participant recruitment and market-appropriate rates, and provided the equivalent of 25 GBP (Great Britain Pound) to GPs answering the survey and 40 GBP to pharmacists. For the general population (denoted as patients) the incentive for survey participation was 0.50–0.75 GBP, which respondents can collect as points for retailer vouchers. We present a descriptive analysis of selected survey questions and provide a list of all questions and answers in the supplementary.
HCP survey
The HCP survey was conducted between 8 November and 22 November 2024. Participants were required to be currently practicing as GP or pharmacist within Switzerland. Due to the inherent difficulty in recruiting licensed HCPs, no strict demographic quotas (e.g. age, gender, region) were applied. Demographic characteristics were collected to ensure broad representation.
HCP participants were recruited from Dynata’s existing verified medical panel. Panel members had previously been profiled according to their medical specialty (GPs or pharmacists), and only those relevant to the study topic were invited for the current survey. The medical panel was established using several recruitment channels, including the purchase of verified contact lists from local medical associations (with prior consent for third-party contact), referrals from existing panelists, as well as professional recruiter networks. All applicants underwent a rigorous verification process prior to inclusion in the panel. This process included submission of a valid medical registration ID, a government-issued form of identification, and contact information. Only after successful verification, individuals were admitted to the medical panel. Data on the HCPs’ preferred language, years in practice, and practice localization (canton) were gathered in the survey.
Patient survey
The parallel patient survey targeted individuals aged ≥ 65 years (at-risk population, as they are recommended annual vaccinations against influenza and COVID-19 at the time of the survey) residing in Switzerland and was conducted between 25 October and 11 November 2024. Enrollment in the patient panel occurred via self-registration through an online form, which was sent to selected people (≥ 65 years) from an already existing panel from Dynata. To verify the authenticity of the applicants, a series of internal validation surveys concerning their medical condition(s) was administered. Only verified individuals were included in the final patient panel, and their preferred language, gender, age, and number of annual doctor visits were inquired. In contrast to the HCP sample, it was more feasible to monitor quotas for gender and language. However, flexibility in age quotas was necessary, given the variability introduced by condition-specific prevalence within the target population.
Results
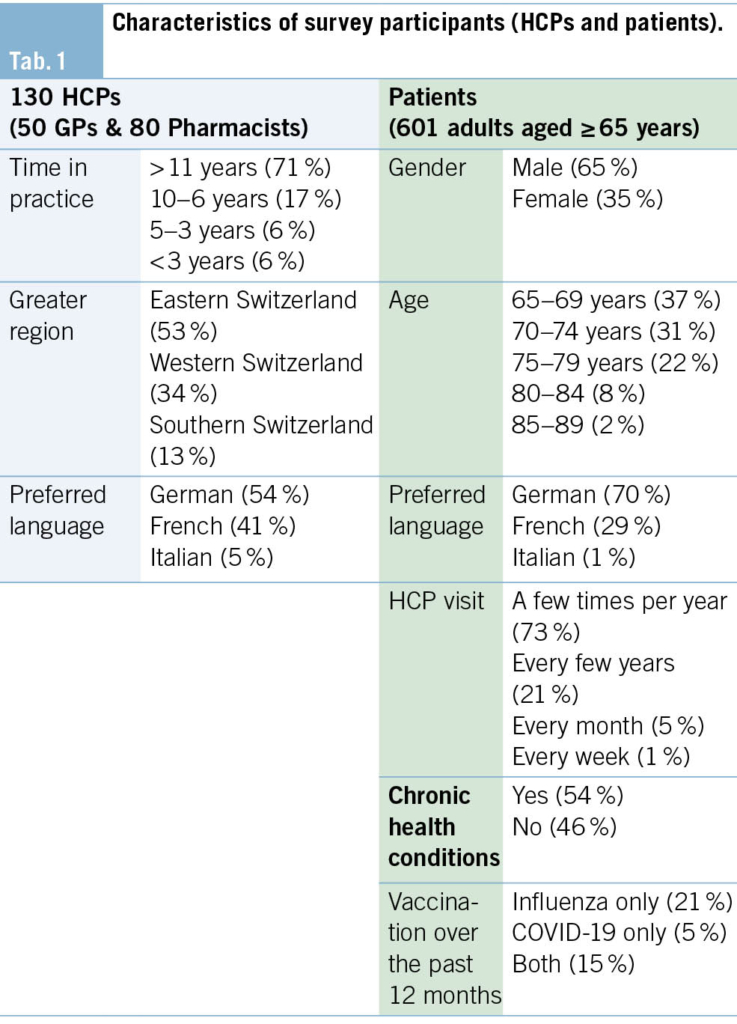
Characteristics of survey participants
In total, 130 HCPs including 50 GPs and 80 pharmacists, as well as 601 adults aged ≥ 65 (patients; at-risk population) filled in the survey (see Tab. 1 for characteristics). The majority of HCPs has been in practice since more than 11 years (71 %), and French speakers were slightly overrepresented in this survey with regards to the overall population in Switzerland (54 % German, 41 % French, 5 % Italian speakers; for detailed regional distribution see suppl. Tab. 1A). In the patient survey, men were overrepresented (65 %), and most patients were between 65–69 (37 %) and 70–74 (31 %) years old. No patient older than 89 years answered the survey. About 70 % of patients gave German as a preferred language (29 % French, and 1 % Italian), and the majority (73 %) consult an HCP a few times per year. More than half of the patients (54 %) indicated having at least one underlying health issue or comorbidity.
Perception of risk by patients
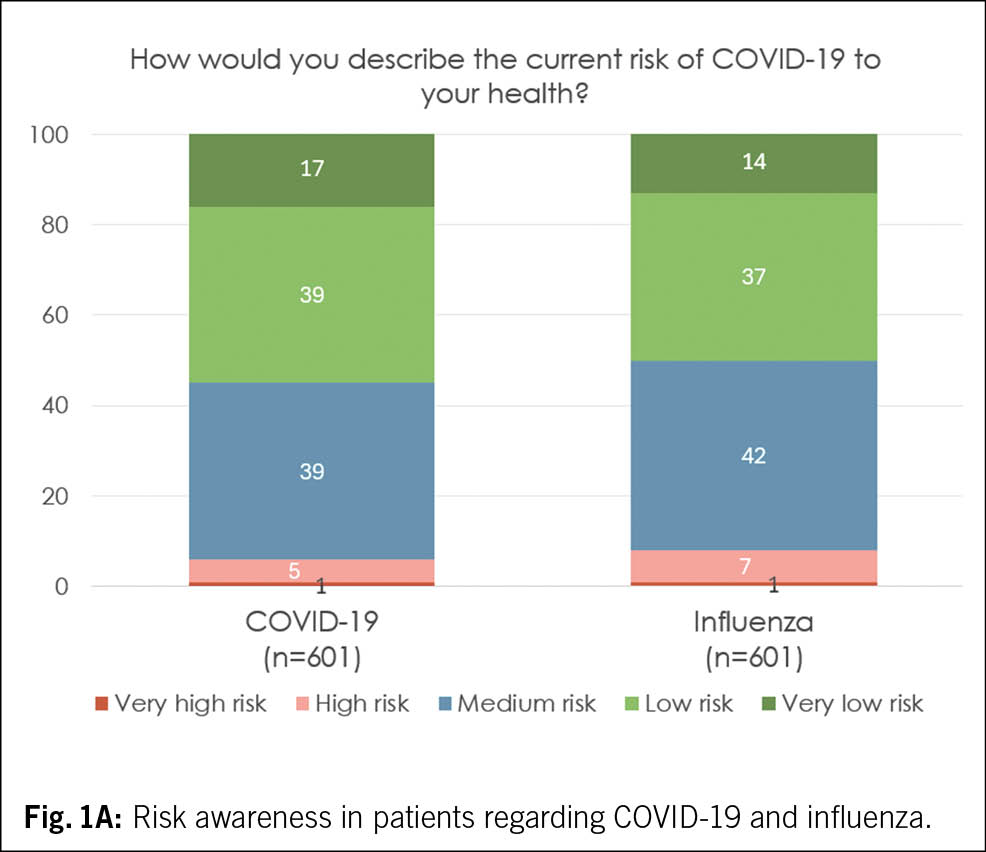
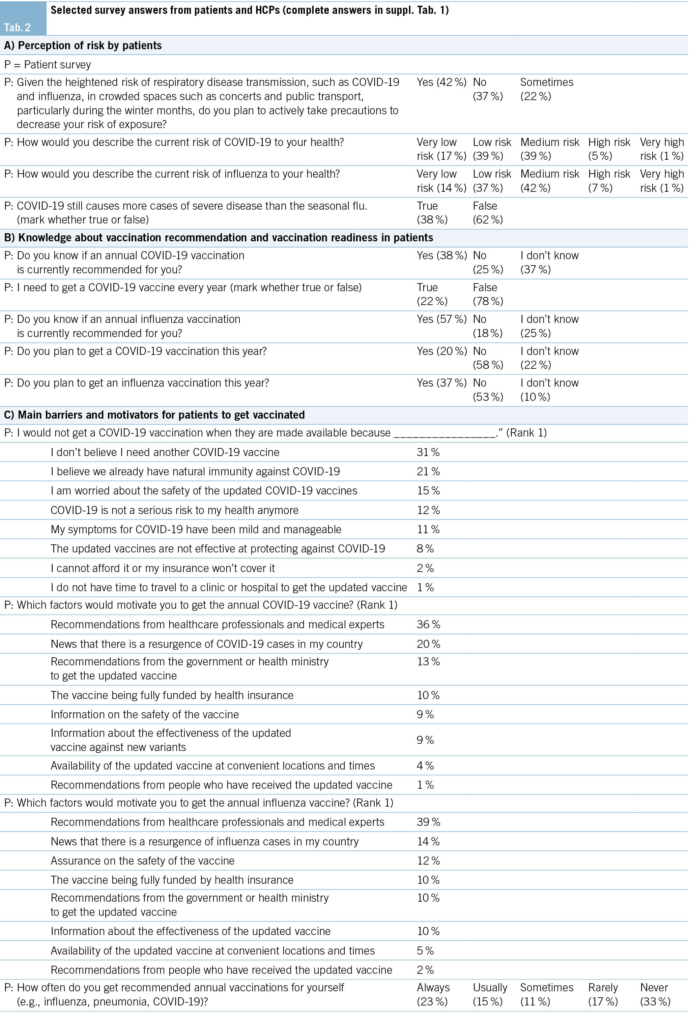
In our survey, 42 % of patients report actively taking precautions to decrease their risk of getting a respiratory infection in general (Tab. 2A). Active precaution was lowest in 65–69-year-old men (34 %), and highest in women above the age of 80 years (67 %, suppl. Tab. 1B). Those who were planning to receive a COVID-19 vaccination or who have had a COVID-19 infection in the past 12 months were more ready to actively take precautions (82 % of 121 patients and 60 % of 62 patients, see suppl. Tab. 1B). Only a minority of patients believe that COVID-19 poses a very high or high risk (6 %) to their health, and most patients (55 %) think that COVID-19 poses a low or even very low risk (Fig. 1A, Tab. 2A). The perception of risk was higher in patients planning to get a COVID-19 vaccine and in those with a COVID-19 infection in the previous 12 months.
Similar trends were visible regarding influenza: About 8 % of patients believe to be at high or very high risk, while the majority (51 %) think that influenza poses a low or very low risk to their health (Fig. 1A, Tab. 2A). However, among women above 80 years, 25 % perceive influenza as a high risk to their health. Also, risk perception is higher in those planning to get a COVID-19 vaccination or those with a recent COVID-19 infection (see suppl. Tab. 1B). As observed in the COVID-19 related-questions, the percentage of people perceiving the virus as a low or very low risk was higher in German speakers compared to French speakers (55 % vs. 41 %).
When asked about the burden of COVID-19 vs. influenza, 38 % of patients answered that they think that COVID-19 causes more cases of severe disease than the flu (Tab. 2A).
Knowledge about vaccination recommendation and vaccination readiness in patients
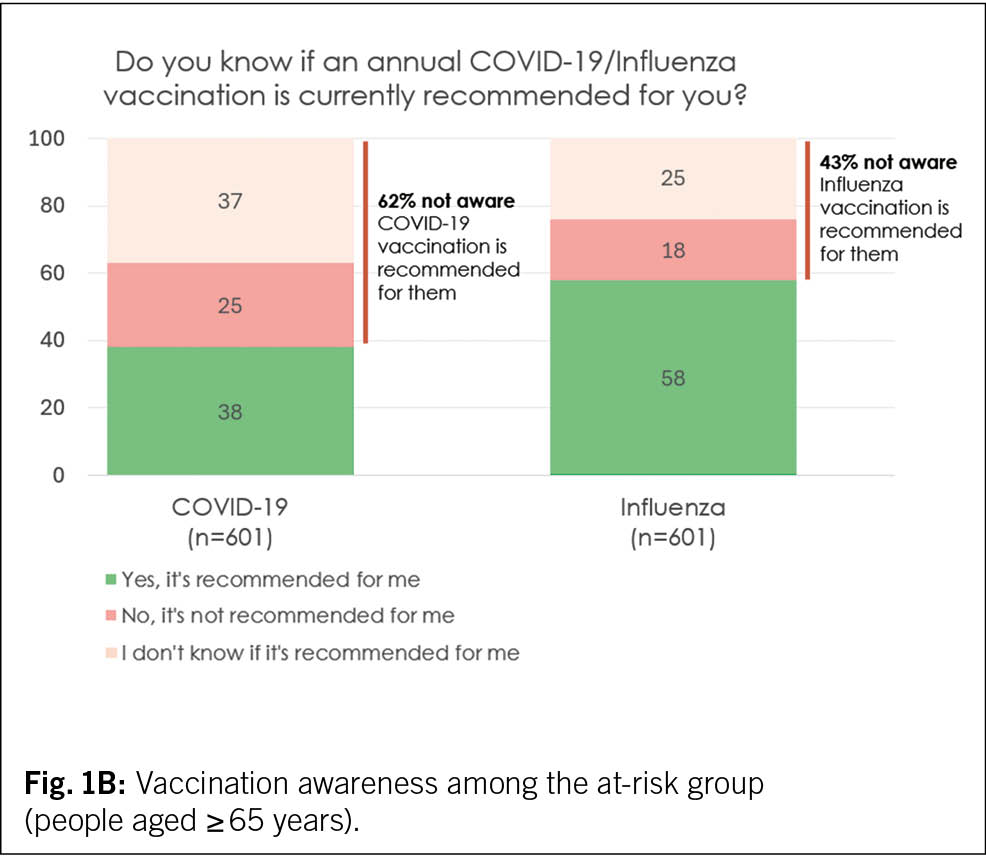
Even though all interviewed patients fall into the at-risk population and are recommended annual COVID-19 and influenza vaccinations by the Swiss authorities and other EU authorities with large public communications, almost two-thirds (62 %) of them are not aware that this is recommended for them: 25 % believe the annual COVID-19 vaccination is not recommended for them, while 37 % are unsure (Fig. 1B, Tab. 2B). Among those who had a COVID-19 infection in the previous 12 months, 60 % knew about the recommendation. Also, awareness of the COVID-19 vaccination recommendation seemed higher in French speakers compared to German speakers (45 % vs. 35 %; suppl. Tab. 1C). When asked whether they need to get a COVID-19 vaccine every year, 78 % of the ≥ 65-year-olds of this survey believed that this was not true (Tab. 2B).
Regarding the annual influenza vaccination, 57 % of the ≥ 65-year-old survey participants knew that it is recommended for them (Fig. 1B, Tab. 2B). Awareness among those with underlying health conditions (n=326) or a COVID-19 infection in the past 12 months was even higher (64 % and 77 %, suppl. Tab. 1C).
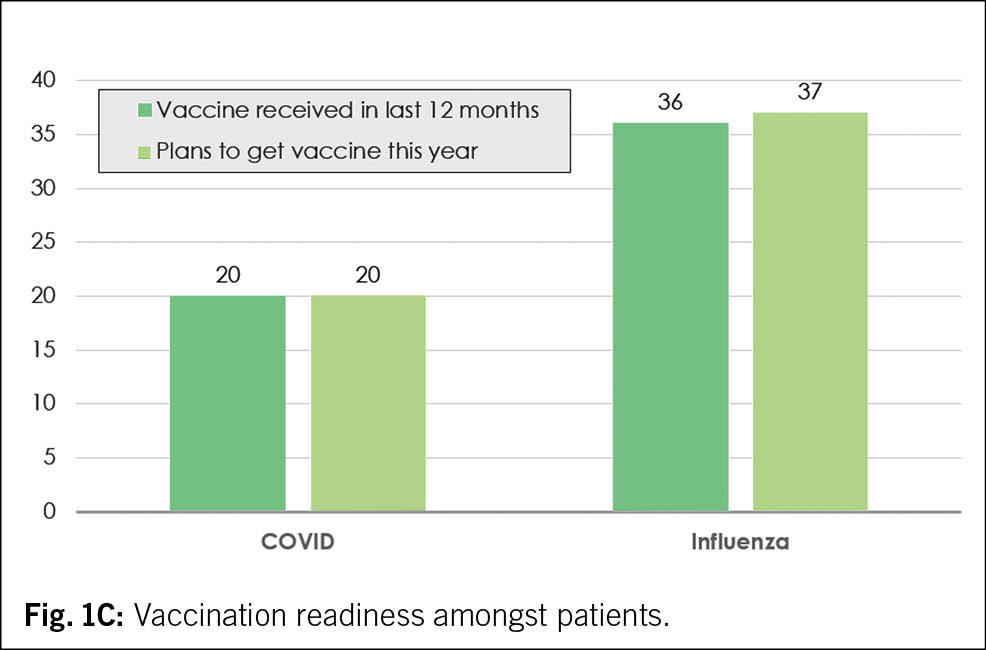
Overall, 41 % of patients had received a COVID-19, influenza or both vaccines in the preceding 12 months (21 % only Influenza; 5 % only COVID; 15 % both), while 59 % did not get any of the vaccines or were not sure if they did (see reported vaccination rates in Tab. 1). Even among those with underlying health conditions, 54 % had not received any vaccination against COVID-19 or influenza in the past 12 months or were not sure. Of all age and gender groups, the 65–69-year-old men (68 %) indicated the lowest vaccination rate (Suppl. Tab. 1A).
20 % of all patients were planning to get the COVID-19 vaccination during the 2024/25 season (Tab. 2B, Fig. 1C). The highest vaccination readiness was found in those aged 80+ (34 %), and the percentage of vaccination readiness was slightly higher in French compared to German speakers (25 % vs. 18 %, suppl. Tab. 1C). However, among those who indicated to have had COVID-19 in the previous 12 months, the readiness for vaccination doubled (40 %, suppl. Tab. 1C).
For influenza, the vaccination readiness was higher in the overall population (37 %) and reached 51 % in those aged 80+ years (Tab. 2B, suppl. Tab. 1C).
Main barriers and motivators for patients to get vaccinated
Among those who were not planning to get a COVID-19 vaccination in 2024/25, the most important reason was that they did not believe they needed another vaccination (31 %) followed by the belief that they already have a natural immunity against COVID-19 (21 %). Moreover, 15 % were worried about the safety of the updated COVID-19 vaccines, with women being more worried than men (Tab. 2C, suppl. Tab. 1D).
The most important motivational factor for patients to get the COVID-19 vaccination was a recommendation by an HCP or medical expert (36 %; Tab. 2C, suppl. Tab. 1D). Similarly, 39 % of patients reported the recommendation of an HCP or medical expert as a main motivator to get the annual influenza vaccination (Tab. 2C, suppl. Tab. 1D). Still, only 38 % of patients in our survey reported to have always or usually received a recommendation for an annual vaccination by an HCP (incl. COVID-19, influenza, and pneumonia) (Tab. 2C, suppl. Tab. 1D). This rate was higher in patients who reported underlying health issues (45 %) and increased with age, reaching 54 % in 80+ year-olds. Still, a third of all survey participants claimed to never have been recommended an annual vaccination.
HCPs knowledge, perception, and attitude towards COVID-19 and its vaccination
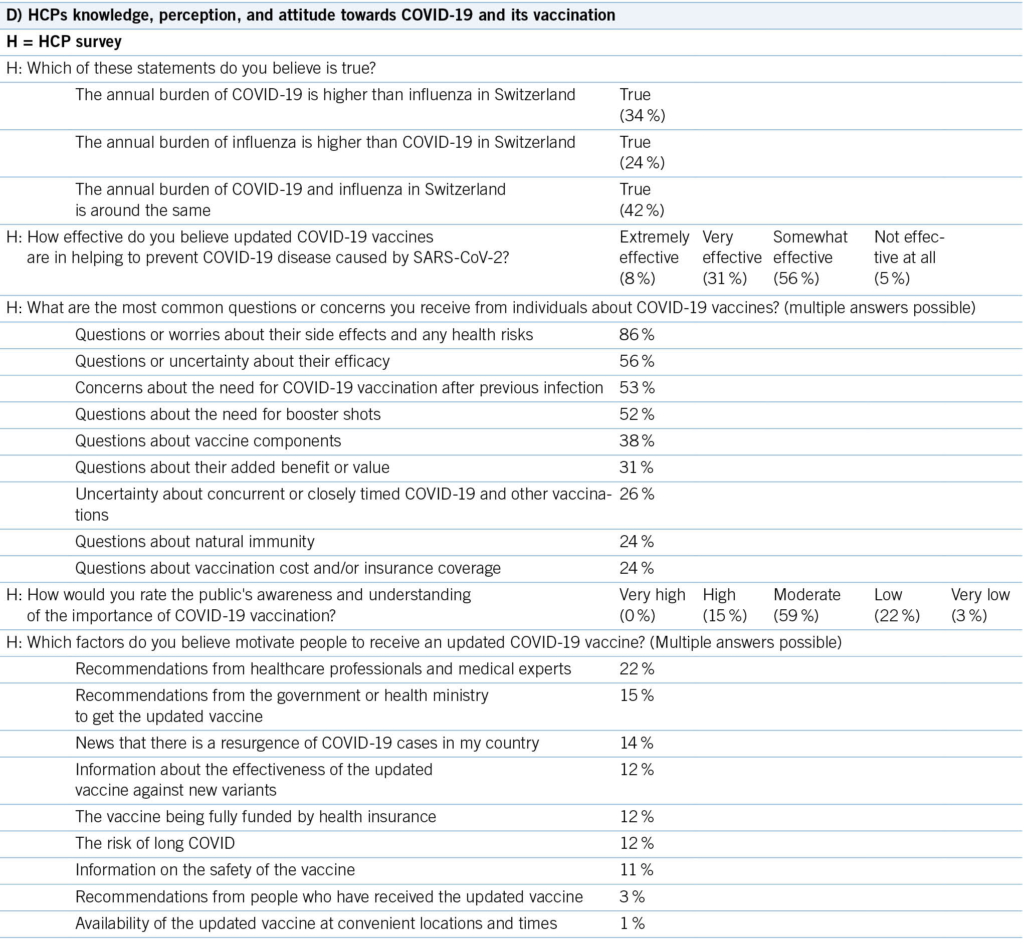
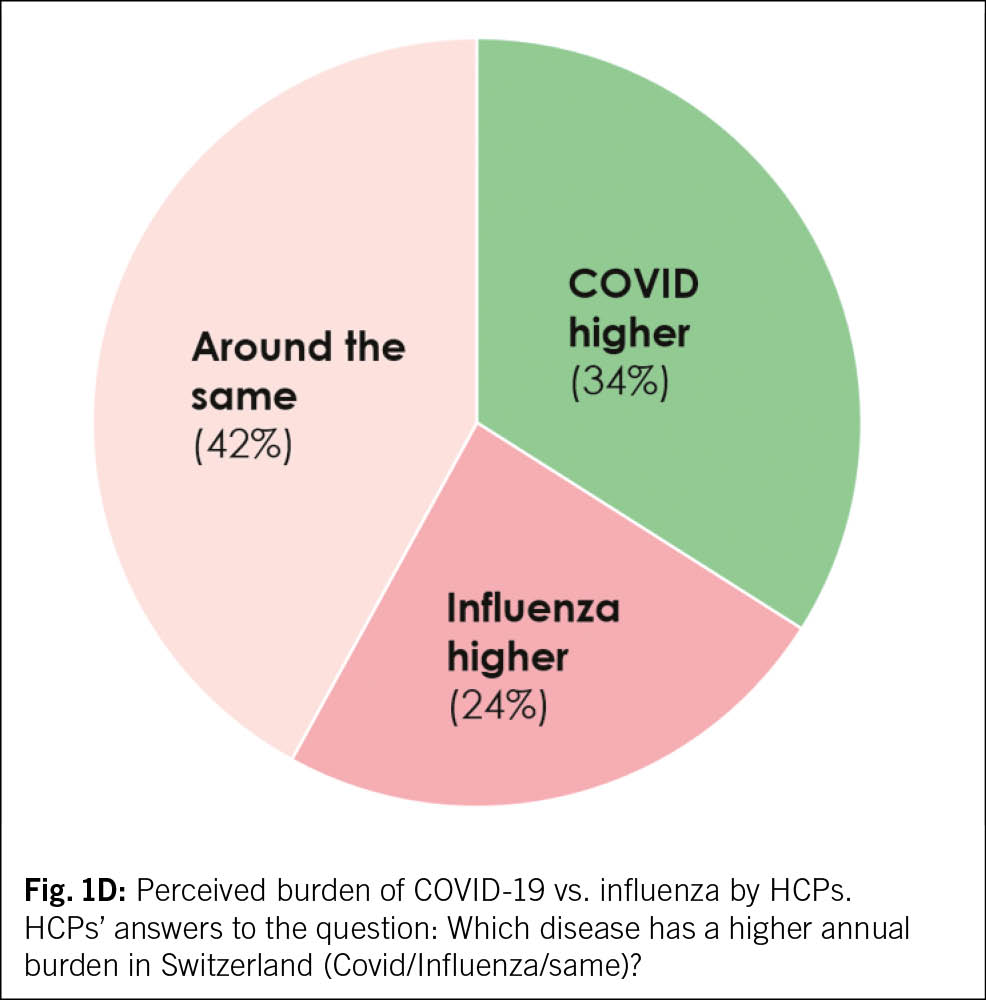
In the season preceding the survey (2023/24), the hospitalization burden with COVID-19 was around 2x higher than with influenza (1). Amongst HCPs, roughly a third were aware of this (34 %), whereas a majority thought that the annual COVID-19 disease burden was lower than for influenza (24 %) or that they were similar (42 %) (Tab. 2D).
Regarding COVID-19 vaccine effectiveness, 56 % of HCPs think that the vaccination is moderately effective and 39 % believe that it is very or extremely effective in preventing COVID-19 disease. Only 5 % of HCPs believe the vaccines are not effective at all (Tab. 2D, suppl. Tab. 1E).
Regarding vaccination barriers, HCPs mainly receive questions and concerns from the public due to worries about side effects and health risks (86 %). They rank the uncertainty about the efficacy as the second biggest concern of the public (56 %) followed by uncertainties about the need for a COVID-19 vaccination after previous infection (53 %) (Tab. 2D). However, HCPs seem to be aware that patients are not informed: a majority of HCPs (59 %) think that the public is only moderately aware of the importance of a COVID-19 vaccine, while 25 % believe that the public has a low or even very low awareness regarding the need for an annual COVID-19 vaccination. French speakers were more aware of the low or very low awareness in the public than German speaking HCPs (31 % vs. 21 %; Tab. 2D, suppl. Tab. 1E).
The most common concerns or questions that HCPs received from patients regarding COVID-19 vaccination were safety-related (86 % reported to receive these questions; Tab. 2D). Other main questions concerned the perceived efficacy (56 %) and the continued need (52 %).
Consistent with patients, HCPs ranked a medical expert’s recommendation as the highest motivator (22 % agreed) for a patient to get vaccinated. HCPs also found recommendations from the government or health ministry (15 %) and news that there is a resurgence of COVID-19 cases in their country (14 %) as important motivators (Tab. 2D).
Discussion
Current vaccination attitudes in the at-risk population and HCPs
At present and at the time of the survey, the Swiss authorities recommend a yearly vaccination against COVID-19 and influenza for people aged ≥ 65 years (3). However, more than half of the respondents believe that COVID-19 and influenza are a low or very low risk to their health, and almost two-thirds are not aware of this recommendation for them. The awareness of the recommendation was slightly better for influenza, with 43 % not being aware. This low awareness of the recommendations is reflected in the low number of people who have received a vaccine in the previous 12 months, and the low readiness to receive a COVID-19 or influenza vaccination in the upcoming season. Similarly low vaccination rates for influenza have been reported in other Swiss studies (8–10). Also, our survey suggests that there are differences in vaccination attitudes depending on age, gender, and region. French speakers were more aware of risks and more open to getting a COVID-19 vaccination than German speakers, even though German and French speakers report similar rates of received vaccination recommendations. Moreover, the awareness of the risks posed by an infection and the readiness to receive a vaccination both increased with age and/or female gender respectively.
Factors influencing vaccination attitudes in the at-risk population
The low awareness of disease risk and vaccination recommendations in the survey participants may be attributed to a lack of targeted and public communication. Indeed, HCPs reported concerns about the safety and efficacy of the vaccines as the most concerning barrier within the public, while patients themselves mostly reported that they just did not feel there was any need for an annual vaccination. While both patients and HCPs ranked the HCPs’ recommendation to get a vaccination as the most important motivator to get vaccinated, only 38 % of all survey participants (patients) reported to have been recommended the annual vaccines regularly. This may not be due to a perceived lack of effectiveness by HCPs, since most HCPs regard the COVID-19 vaccination as at least somewhat effective in preventing disease. Also, it can be hypothesized that the perceived effectiveness regarding the prevention of severe forms of the disease may have been even higher. Thus, infrequent primary care consultations may partly explain the observed low vaccination coverage, as the frequency of seeing a GP has previously been linked to a higher likelihood of getting the influenza vaccine (8). Since older patients might see the GP more often, they may develop a higher awareness regarding disease risk and recommended vaccinations.
HCPs listed safety concerns as the major question or concern they hear from patients (86 %). Surprisingly, amongst patients who do not plan to get vaccinated in the upcoming season, only 15 % reported safety concerns as a reason, whereas questioning the continued need for vaccination was listed much more often.
Limitations of the survey
First, selection bias is likely, as individuals who are more health-conscious or vaccine-accepting may be more inclined to participate in such a survey, which could lead to an overestimation of vaccine willingness. This bias would thus be conservative in nature. Against this background, vaccine-hesitant or critical attitudes may even be underestimated in the dataset and could be more pronounced in the general population. This may in part be reflected in the discrepancy between the readiness to receive a COVID-19 vaccination in 2024/25 (20 % in our survey) and our estimated true vaccination rate in that season (12 %) (13). Additionally, more men (65 %) than women answered the patient survey. Since women had different perceptions regarding the risk of infections, taking precautions, and the safety of the vaccine, this may slightly shift the overall outcome in favor of men’s attitudes.
Potential strategies to address risk perception and awareness of recommendations
According to our survey, informing the public on disease burden and vaccination recommendations should be a priority to close the apparent knowledge gap in the public and to relieve the burden on hospitals. Since vaccination rates are typically much higher in children than in adults (16), a similarly clear agenda might help adults to keep regular vaccination check-ups to prevent short term but also long-term disease and complications. Encouraging and funding systematic checking of the vaccination status in people at risk by HCPs and educating people on the burden of infectious diseases may be important in the implementation of such strategies. Additionally, the inclusion of vaccination as a preventive measure in school curricula may already raise awareness at an earlier age. Also, public mass campaigns by health authorities can be very effective (17). Some cantons have already set up campaigns (e.g. https://www.be-impft.ch/, https://www.sg-impft.ch/) and the FOPH has implemented an integrated respiratory disease campaign covering COVID-19, influenza, and RSV for the first time in the season of 2025/26 (3). The introduction of the exemption from the deductible for all recommended vaccines as well as time used for vaccination advice as of 2026 may further decrease existing barriers.
Conclusions
Our survey among people aged 65 years and older in Switzerland revealed low risk perception of viral respiratory diseases, and low awareness of vaccination recommendations. Recommendation by an HCP appears as a major driver of communicating vaccination recommendations to people at-risk (8). Thus, it may be advisable for GPs and pharmacists to adopt more proactive outreach strategies during the respiratory season, particularly targeting EKIF-defined risk groups (e.g., individuals aged ≥ 65 years), and to engage them in discussions regarding their vaccination status.
Philippe Eggimann 1, Thomas Steffen 2, Daphne McCarthy-Pontier 3, Thomas Rosemann 4
1 Medical Society of French-speaking Switzerland, Fribourg, Switzerland
2 Steffen Consulting GmbH, Basel, Switzerland
3 Medical Affairs, Moderna Switzerland GmbH, Basel, Switzerland
4 Institut für Hausarztmedizin, Universitätsspital Zürich, Switzerland
Abbreviations
COVID-19 coronavirus disease 2019
EKIF Federal Commission for Vaccinations (Eidgenössische Kommission für Impffragen)
FOPH Swiss Federal Office of Public Health
GP general practitioner
HCP health care professional
RSV respiratory syncytial virus
WHO World Health Organization
History
Manuscript received: 18.12.2025
Accepted after revision: 22.04.2026
Supplementary Materials online at
https://www.hausarztmedizin.uzh.ch/de/vaccination
Institut für Hausarztmedizin
Universitätsspital Zürich
Pestalozzistrasse 24
8091 Zürich
thomas.rosemann@usz.ch
The study was initiated, designed and funded by Moderna. Authors PE, TS and TR received financial compensation from Moderna Switzerland GmbH for the analysis of the data and manuscript preparation. DM is an employee and shareholder of Moderna. The content reflects the author’s independent analysis and interpretation. The manuscript was prepared by Iaculis GmbH in Zurich, Switzerland.
• Both patients and HCPs underestimate the burden of COVID-19 compared to influenza.
• Awareness of the annual COVID-19 and influenza vaccination recommendations among people aged ≥ 65 years is low.
• The fact that people aged ≥ 65 years do not think they need another vaccination appears as a key vaccination barrier.
• HCP recommendation is the strongest motivator for vaccination in people aged ≥ 65 years.
1. COVID-19 and Influenza Hospital Based Surveillance (CH-SUR). Bericht zum spitalbasierten Covid-19- und Grippe-Sentinel Überwachungssystem Woche 20/2024. Available at: https://www.bag.admin.ch/de/respiratorische-viren# %C3 %9Cberwachung-von-Covid-19-und-Grippe-in-Schweizer-Spit %C3 %A4lern-; last accessed August 2025.
2. Lorenz, N., et al., Decline of antibodies to major viral and bacterial respiratory pathogens during the COVID-19 pandemic. J Infect Dis, 2024.
3. Bundesamt für Gesundheit (BAG) & Eidgenössische Kommission für Impffragen (EKIF). Schweizerischer Impfplan 2026. Available at: https://www.bag.admin.ch/de/schweizerischer-impfplan; last accessed April 2026.
4. État de Vaud. Des opérations électives sont reportées en raison d’une forte surcharge. Publié le 29 janvier 2025. https://www.vd.ch/actualites/communiques-de-presse-de-letat-de-vaud/detail/communique/des-operations-electives-sont-reportees-en-raison-dune-forte-surcharge; last accessed August 2025.
5. Baxter, R., G.T. Ray, and B.H. Fireman, Effect of influenza vaccination on hospitalizations in persons aged 50 years and older. Vaccine, 2010. 28(45): p. 7267-72.
6. Lin, D.Y., et al., Durability of XBB.1.5 Vaccines against Omicron Subvariants. N Engl J Med, 2024. 390(22): p. 2124-2127.
7. Current product information available at www.swissmedicinfo.ch.
8. Plate, A., et al., Influenza vaccination uptake among at-risk patients in Switzerland-The potential of national claims data for surveillance. Influenza Other Respir Viruses, 2023. 17(10): p. e13206.
9. Plate, A., et al., Influenza vaccination patterns among at-risk patients during the Covid-19 pandemic-a retrospective cross-sectional study based on claims data. Infection, 2024. 52(4): p. 1287-1295.
10. Bundesamt für Gesundheit (BAG). Saisonale Grippe und Grippeimpfung 2023/2024. BAG Bulletin 41 2023. Available at: https://www.infovac.ch/docs/public/influenza/saisonale-grippe-und-grippeimpfung-2023-2024-.pdf; last accessed August 2025.
11. World Health Organization (WHO). Managing seasonal vaccination policies and coverage in the European Region. Available at: https://www.who.int/europe/activities/managing-seasonal-vaccination-policies-and-coverage-in-the-european-region?utm_source=chatgpt.com; last accessed August 2025.
12. European Center for Disease Control and Prevention (ECDC), Survey report on national seasonal influenza vaccination recommendations and coverage rates in EU/EEA countries. Available at: https://www.ecdc.europa.eu/en/publications-data/survey-report-national-seasonal-influenza-vaccination-recommendations; last accessed August 2025. 2024.
13. IQVIA MIDAS® Monthly sales volume data for Switzerland; Data period: September 2024 to December 2024; Market definition: International products COMIRNATY and SPIKEVAX, each as estimates of real market activity. Copyright IQVIA. All rights reserved.
14. European Center for Disease Control and Prevention (ECDC), COVID-19 vaccination coverage in the EU/EEA during the 2023–24 season campaigns, 1 September 2023 – 31 July 2024; Available at: https://www.ecdc.europa.eu/en/publications-data/covid-19-vaccination-coverage-eueea-during-2023-24-season-campaigns-1-september; last accessed August 2025. 2024.
15. Dynata, https://www.dynata.com/; last accessed August 2025.
16. Federal Office of Public Health (FOPH). BAG Bulletin 13/24. Available at: https://www.bag.admin.ch/de/bag-bulletin; last accessed August 2025.
17. Dubé, E., D. Gagnon, and N.E. MacDonald, Strategies intended to address vaccine hesitancy: Review of published reviews. Vaccine, 2015. 33(34): p. 4191-203.
PRAXIS
- Vol. 115
- Ausgabe 5
- Mai 2026